Introduction: The Invisible Threat to Vision
Glaucoma is often referred to by ophthalmologists as the “silent thief of sight.” This moniker is well-earned. Unlike many other ocular conditions that present with redness, itching, or sudden blurring, glaucoma frequently develops with zero warning signs. In a bustling tech hub like Bangalore, where thousands of professionals spend 10+ hours a day staring at digital screens, the subtle onset of glaucoma is easily dismissed as simple “eye strain” or “tiredness.”
The Anatomy of the Eye: Understanding the “Drainage System”
To understand why glaucoma is so dangerous, one must understand how the eye maintains its shape and health. The front of the eye is filled with a clear fluid called aqueous humor. This isn’t the same as tears; it’s an internal fluid that provides nutrients to the eye.
The Inflow-Outflow Balance
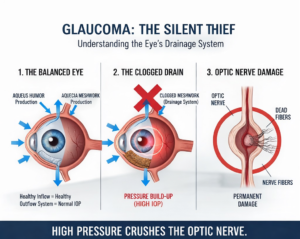
The eye is constantly producing this fluid. To maintain a steady internal pressure (Intraocular Pressure or IOP), an equal amount of fluid must drain out through a microscopic drainage system called the trabecular meshwork, located at the angle where the iris and cornea meet.
When the Drain Fails: If the drainage angle becomes blocked or the meshwork becomes “clogged” (common in aging populations), the fluid builds up.
The Pressure Cooker Effect: This build-up creates pressure that pushes backward against the most vulnerable part of the eye: the Optic Nerve.
Nerve Death: The optic nerve is made of over a million tiny nerve fibers. As pressure rises, these fibers begin to die. Once a nerve fiber dies, it cannot be regenerated. This is why glaucoma vision loss is permanent.
The Different Types of Glaucoma
While most people think of glaucoma as a single disease, it is actually a spectrum of conditions. At Move and Shine Eye Clinic, we categorize them to provide targeted treatment.
1. Primary Open-Angle Glaucoma (POAG)
This is the most common form in India. The drainage angle remains “open,” but the fluid passes too slowly. It’s like a kitchen sink where the pipe is slightly narrowed; it drains, but not fast enough to prevent a backup.
Symptoms: None in the early stages.
Progression: Very slow, often taking years to notice.
2. Angle-Closure Glaucoma (ACG)
This is more common in Asian eyes due to slightly different ocular anatomy (shallower anterior chambers). The iris can literally “slide” over the drainage angle and shut it off completely.
- Acute ACG: A sudden total blockage. This is a medical emergency. Symptoms include intense eye pain, nausea, vomiting, and seeing “halos” around lights.
- Chronic ACG: The angle closes slowly over time without pain.
3. Normal-Tension Glaucoma (NTG)
This is a diagnostic challenge. The patient’s eye pressure is within the “normal” range (typically 12-21 mmHg), yet the optic nerve still shows damage. This is often linked to poor blood flow to the eye, frequently seen in patients with low blood pressure or migraines.
4. Secondary Glaucomas
These are caused by external factors or underlying health issues:
Steroid-Induced: Misuse of over-the-counter “cooling” eye drops containing steroids.
Pseudoexfoliation: A condition where flake-like deposits clog the drain.
Neovascular: Often caused by advanced Diabetes, where new blood vessels grow over the drainage angle.

Why We Are at Risk
The IT Professional & Digital Strain
While screen time doesn’t directly cause glaucoma, the “Digital Lifestyle” often masks it. Professionals in Bangalore often ignore “peripheral shadows” or “occasional blurriness,” attributing it to 12-hour shifts. Furthermore, high myopia (nearsightedness) is becoming an epidemic among young urbanites, and high myopes are at a much higher risk for glaucoma.
The Diabetes Capital
India is often cited as the diabetes capital of the world. High blood sugar levels can lead to the growth of abnormal blood vessels that block the eye’s drainage system, leading to aggressive forms of the disease.
The “Silent” Family History
Many families do not discuss medical histories openly. If your parents or grandparents had “vision loss in old age,” it might not have been just cataracts—it might have been undiagnosed glaucoma. Because it is hereditary, this puts the next generation at extreme risk.
What to Expect at Move and Shine?
A “standard” eye test for glasses is not a glaucoma screening. We utilize specialized diagnostic tools:
Applanation Tonometry: Using the Goldmann Applanation Tonometer, we gently touch the numbed surface of the eye to get the most precise pressure reading available today.
Gonioscopy: We use a specialized mirrored lens to look inside the eye’s drainage angle. This determines if you have “Open” or “Closed” angle glaucoma.
Pachymetry: A thin cornea can make your eye pressure look “normal” even when it is dangerously high. We measure corneal thickness to adjust your IOP readings for 100% accuracy.
OCT (Optical Coherence Tomography): This is our “early warning system.” The OCT provides a microscopic, 3D map of the Retinal Nerve Fiber Layer (RNFL), detecting thinning up to 5 years before symptoms appear.
Visual Field Analysis (Perimetry): This computer-assisted test measures your “side vision” and maps out blind spots.

Treatment Milestones: Life After Diagnosis
Receiving a glaucoma diagnosis can be scary, but with modern medicine, blindness is almost entirely preventable.
Phase 1: Medicated Eye Drops
For 80% of patients, a single daily drop is enough. These drops either slow down fluid production or open up the “pipes” to increase drainage. Consistency is key.
Phase 2: Laser Therapy (SLT)
Selective Laser Trabeculoplasty (SLT) is a revolutionary “cold” laser treatment. It is painless, takes 5 minutes, and can sometimes eliminate the need for daily eye drops for several years.
Phase 3: Surgical Intervention
If medications and lasers aren’t enough, we perform Trabeculectomy or implant MIGS (Minimally Invasive Glaucoma Surgery) devices to create a “permanent bypass” for the fluid.
Nutrition and Lifestyle: Supporting Your Treatment
While no diet can “cure” glaucoma, supporting vascular health is essential for protecting the optic nerve. This aligns with the mission of Precimax Life Sciences, where we emphasize evidence-based, targeted nutraceuticals to mitigate health risks.
The Glaucoma-Friendly Diet
Nitrate-Rich Greens: Spinach, kale, and collard greens can reduce POAG risk by 20-30% by improving blood flow.
Omega-3 Fatty Acids: Found in flaxseeds, walnuts, and fatty fish; these help reduce ocular inflammation.
Anthocyanins: Found in dark berries (blueberries, blackberries), these strengthen the blood-brain-eye barrier.
Lifestyle Adjustments
The Yoga Factor: Avoid inverted poses (like Headstands) which increase eye pressure. Keep your head above your heart.
Hydration: Sip water throughout the day. “Chugging” a liter of water can cause temporary pressure spikes.
Sleep: Use a thicker pillow to sleep at a 20-30 degree incline, which helps lower nocturnal eye pressure.
Expert Commentary: Insights from Dr. Dona Susan
On Early Detection: “I often see patients who come in for a routine ‘power check’ for new glasses, only for us to discover advanced glaucoma. In Bangalore, we need to shift the culture from ‘corrective’ care to ‘preventive’ care.”
On Medication Adherence: “The biggest challenge isn’t the science; it’s the schedule. You must treat your eye drops like a lifeline.”
On Family Screenings: “One person’s diagnosis can be the ‘warning bell’ that saves the sight of five others.”
Frequently Asked Questions (FAQs)
1. Is eye pressure the only indicator of glaucoma?
No. Some people have “Normal-Tension Glaucoma” where they lose vision at “normal” pressure. The health of the optic nerve is the ultimate indicator.
2. Can I wear contact lenses if I have glaucoma?
Yes, but wait 15 minutes after applying drops before inserting lenses, or use preservative-free drops to avoid lens damage.
3. Does stress cause glaucoma?
Stress causes temporary spikes in pressure but isn’t a direct cause. However, managing stress helps overall ocular health.
4. Can I drive if I have glaucoma?
In early stages, yes. In advanced stages, peripheral vision loss and glare can make night driving dangerous. Regular testing is required to monitor safety.
5. Is the damage from glaucoma reversible?
No. Optic nerve fibers cannot be regenerated. Early detection is the only way to save remaining vision.
6. Can children get glaucoma?
Yes, though rare, “Pediatric Glaucoma” exists and requires immediate specialist intervention.
7. Is glaucoma surgery painful?
Most procedures are performed under local anesthesia with minimal discomfort and a relatively quick recovery time.
8. Can I use “cooling” eye drops for redness?
Be careful. Some contain steroids which, if used long-term, can cause Steroid-Induced Glaucoma. Always consult a doctor first.
9. How often should I get screened?
If you are over 40 or have a family history, an annual comprehensive eye exam is highly recommended.
10. Does coffee increase eye pressure?
Caffeine can cause a slight, temporary increase in IOP. Moderate consumption is usually fine, but avoid excessive intake.
11. Can exercise help?
Moderate aerobic exercise (walking, swimming) can actually help lower eye pressure. Avoid heavy weightlifting that involves “straining” or holding your breath.
12. Is glaucoma related to high blood pressure?
There is a link. Very high BP can increase eye pressure, but very low BP can reduce blood flow to the optic nerve. Balance is key.
13. Will I go blind if I have glaucoma?
With early detection and strict adherence to treatment, the vast majority of patients maintain functional vision for their entire lives.
14. What is the difference between Glaucoma and Cataracts?
Cataracts are a clouding of the lens (reversible with surgery). Glaucoma is nerve damage (permanent). You can have both at the same time.
15. Are there natural supplements for glaucoma?
Certain antioxidants and neuroprotective compounds (like those researched by Precimax Life Sciences) can support nerve health, but they supplement—rather than replace—prescribed drops.
16. Why do my eye drops sting?
Some medications or their preservatives can cause mild stinging. If it persists, ask your doctor about preservative-free alternatives.
17. Can I still play sports?
Yes, but use protective eyewear, especially for racquet sports, as eye trauma can cause secondary glaucoma.
18. Does smoking affect glaucoma?
Yes. Smoking increases oxidative stress and affects blood flow to the eye, worsening the progression of the disease.
19. Is there a “cure” on the horizon?
Research into stem cells and gene therapy is ongoing, but currently, the only proven “cure” is prevention and management.
20. Why choose Move and Shine Eye Clinic?
We provide continuity of care, advanced micron-level imaging, and a holistic approach that looks at your lifestyle, not just your eyes.
Conclusion: Your Vision is Your Future
In a city as vibrant as Bangalore, vision is our most valuable asset. It allows us to navigate the traffic, excel in our careers, and enjoy the greenery of Cubbon Park. Don’t let the “Silent Thief” take that away from you.




