As we observe World Obesity Day 2026, the medical community is moving toward a more profound understanding of excess weight. At Move and Shine Orthopedic Wellness & Eye Clinic, we no longer view obesity simply through the lens of body mass index (BMI) or aesthetics. Instead, we recognize it as a systemic inflammatory condition—a chronic state of metabolic “fire” that prematurely ages the human body from the delicate layers of the retina to the resilient cushions of the knee cartilage.
In India, the transition to an urban, sedentary lifestyle has accelerated a health crisis. We are seeing a “compositional shift” where lower baseline muscle mass combined with higher visceral fat is triggering joint degeneration and metabolic eye diseases in patients as young as their early 30s. This blog explores the critical link between weight, musculoskeletal integrity, and ocular health, championing a philosophy of preservation over replacement.
Obesity is Not Just About Size – The Systemic Threat
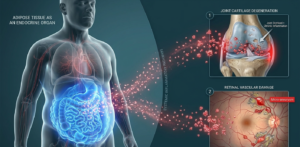
The narrative surrounding weight is often oversimplified. However, in 2026, clinical evidence is clear: obesity is an active, aggressive biological state. Adipose (fat) tissue acts as an endocrine organ, secreting pro-inflammatory chemicals known as adipokines (such as leptin and interleukin-6).
These chemicals don’t just stay in the fat cells; they travel through the bloodstream, weakening the structural integrity of:
Cartilage: Accelerating the breakdown of the smooth surfaces in our joints.
Tendons and Ligaments: Reducing their elasticity and making them prone to tears.
The Retina: Damaging the microscopic blood vessels that allow us to see.
At Move and Shine, we bridge the gap between orthopedics and ophthalmology. We see the daily impact of this systemic inflammation—where a patient presenting with early-stage knee osteoarthritis often shows early markers of metabolic retinal stress.
India’s Changing Body Composition – The “Early Onset” Crisis
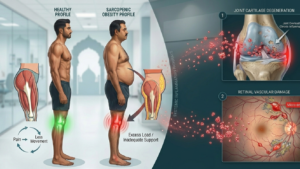
India faces a unique challenge known as the “Thin-Fat Phenotype.” Many Indian adults appear relatively lean but possess a high percentage of visceral fat and dangerously low skeletal muscle mass. This lack of “muscle armor” leaves our joints exceptionally vulnerable.
The New Clinical Reality:
The 30s Crisis: We are increasingly treating young professionals for lumbar disc herniations and chronic back pain caused by poor core stability and abdominal weight.
Early Knee OA: Knee Osteoarthritis, once a disease of the 60s, is now prevalent in the 40s.
Overuse Injuries: We see a rise in Achilles tendinopathy and plantar fasciitis in individuals who attempt sudden “weekend warrior” activities without the muscular strength to support their weight.
Orthopedic Consequences of Excess Weight
The physics of obesity are unforgiving. Every movement involves a “load amplification” effect.
1. Knee Joint Degeneration
When you walk, the pressure across your knees is 3 to 4 times your total body weight. For every 5 kg of excess weight, you are adding 15–20 kg of extra pressure to your knees with every single step. This constant grinding leads to the early death of chondrocytes (cartilage cells).
2. Spine and Disc Degeneration
The lumbar spine (lower back) acts as the body’s primary crane. Excess abdominal weight shifts the center of gravity forward, causing an anterior pelvic tilt. This creates uneven axial loading on the spinal discs, leading to premature “wear and tear,” stiffness, and nerve impingement.
3. The Ankle and Foot: The Foundation
Your feet are the first point of contact with the earth. Obesity is a primary driver for:
Plantar Fasciitis: Inflammation of the thick band of tissue across the bottom of the foot.
Flat Foot Progression: The arches literally collapse under sustained weight, leading to a chain reaction of pain up to the hips.
4. The Inflammatory Weakening of Tendons
Beyond the mechanical load, adipokines actively inhibit the repair mechanisms of tendons. This is why overweight individuals often suffer from chronic tendon issues like “Tennis Elbow” or “Achilles Tendonitis,” even without engaging in high-intensity sports.
Obesity in Sports and Active Individuals
At Move and Shine, we apply Sports Medicine principles to all patients, regardless of their athletic level. In an overweight individual, the risk of acute injury is significantly higher.
ACL Risk: Higher body mass index is statistically linked to non-contact ACL tears because the muscles cannot stabilize the joint during sudden pivots.
Slower Recovery: Inflammation slows down the healing of soft tissues. A minor sprain that takes a lean athlete one week to heal might take an overweight individual three weeks.
Weight optimization is the most effective “protective gear” an athlete can wear.
Joint Preservation vs. Joint Replacement
A core mission of our clinic is to move away from the “wait and replace” model. For a patient in their 40s or 50s, a total joint replacement should be the last resort, as the lifespan of an implant is finite.
Our Joint Preservation Strategies Include:
Regenerative Medicine: Using PRP (Platelet-Rich Plasma) and cellular therapies to stimulate the body’s own healing.
Alignment Correction: Using specialized bracing and physical therapy to shift weight away from the damaged side of the joint.
Targeted Strengthening: Building the quadriceps and glutes to act as biological “shock absorbers.”
Key Point: Joint preservation is only successful if the underlying mechanical stress (weight) is managed.
Why Weight Optimization Before Regenerative Procedures Matters
Many patients come to us asking for “the magic injection” (PRP or Stem Cell therapy). While these treatments are revolutionary, their efficacy is directly tied to the patient’s metabolic health.
Why weight loss must come first (or coincide):
Lowering the “Inflammatory Soup”: If the joint environment is highly inflammatory due to obesity, the injected growth factors will be “neutralized” before they can heal the cartilage.
Mechanical Integrity: It is counterproductive to repair cartilage only to continue crushing it under excessive load.
Better Outcomes: Clinical data shows that patients who lose even 5–7% of their body weight before a PRP procedure report 40% higher satisfaction and longer-lasting pain relief.
Post-Procedure Maintenance – Preventing the Reversal
After a successful regenerative procedure, the work isn’t over. Weight regain can quickly reverse the biological gains made during therapy. We implement Structured Rehab Programs that focus on:
Core Stability: Protecting the spine.
Proprioception: Improving the brain-body connection so you don’t re-injure the joint.
Inflammatory Monitoring: Periodically checking markers like CRP to ensure the body remains in a “healing state.”
GLP-1 Analogues – A Balanced Orthopedic Perspective
The rise of GLP-1 medications (like Semaglutide) has changed the weight loss landscape in 2026. While they are highly effective for weight reduction, they carry a hidden risk: Muscle Wasting (Sarcopenia).
If a patient loses 15 kg but 5 kg of that is muscle, their joints actually become less stable. At Move and Shine, we advocate for:
Protein-Sparing Weight Loss: Ensuring high protein intake during medication use.
Resistance Training: Essential to signal the body to keep its muscle while losing fat.
Weight loss is only a “win” if your muscles remain strong enough to protect your bones.
Sustainable Weight Reduction Framework
We don’t believe in “crash diets.” We believe in metabolic flexibility. Our framework includes:
High Protein Intake: 1.2g to 1.5g of protein per kg of body weight to preserve lean mass.
Micronutrient Correction: Addressing Vitamin D and B12 deficiencies, which are rampant in India and critical for muscle function.
Sleep Hygiene: Lack of sleep increases cortisol, which drives abdominal fat storage and joint inflammation.

Role of Structured Meal Replacements (SMRs)
For patients with severe joint pain who cannot exercise intensely, Structured Meal Replacements provide a “metabolic reset.”
Calorie Control: Eliminates the guesswork and “portion creep.”
Nutrient Density: Provides the building blocks (amino acids/vitamins) needed for joint repair while maintaining a calorie deficit.
The Hidden Connection – Obesity and Eye Health
This is where Move and Shine offers a unique perspective. Obesity isn’t just a threat to your ability to walk; it is a threat to your ability to see.
The Metabolic Link to Vision:
Diabetic Retinopathy: Obesity is the primary driver of Type 2 Diabetes. High blood sugar damages the tiny blood vessels in the retina, leading to leakage and potential blindness.
Hypertensive Retinopathy: Excess weight raises blood pressure, which can cause the retinal vessels to thicken and narrow, restricting blood flow to the optic nerve.
Glaucoma Risk: Recent studies suggest that metabolic syndrome can increase intraocular pressure, a major risk factor for glaucoma.
Macular Edema: Chronic systemic inflammation contributes to fluid buildup in the macula, the part of the eye responsible for sharp, central vision.
Protecting your metabolism is synonymous with protecting your vision.
The Integrated “Move and Shine” Approach
We believe that the eye and the knee are connected by the same blood and the same metabolism. Our integrated care model includes:
Body Composition Evaluation: Using advanced scans to see fat vs. muscle.
Metabolic Eye Screening: Annual retinal exams for any patient with a BMI over 27.
Sports Medicine Consultation: Creating movement plans that don’t hurt.
Preventive Strategy for 40+ Adults
If you are over 40, we recommend an annual “Wellness Audit”:
Joint Mobility Check: Identifying early “stiff zones.”
HbA1c & Lipid Profile: Monitoring the “internal fire.”
Digital Retinal Imaging: Catching microvascular changes before they affect vision.
Muscle Strength Assessment: Ensuring you have the “armor” to protect your aging skeleton.
Long-Term Maintenance – Consistency Over Intensity
The secret to health in 2026 is not a 30-day challenge; it is the daily accumulation of small wins.
Strength Training: Twice a week for life.
Anti-Inflammatory Nutrition: Prioritizing whole foods over processed ones.
Periodic Rehab: Seeing a specialist before the “ache” becomes a “tear.”

Call to Action – Reclaim Your Future
This World Obesity Day 2026, don’t just weigh yourself—assess yourself. Are your joints supporting your movement? Is your metabolism protecting your vision?
At Move and Shine Orthopedic Wellness & Eye Clinic, we are here to help you optimize your weight, preserve your joints, and safeguard your sight. Movement is the foundation of life. Vision is the window to it. Let’s protect both.
FAQs: Obesity, Joint Health, and Vision
1. Why does my back hurt more when I gain weight?
Excess weight, especially in the abdomen, pulls your spine forward, putting constant strain on your lower back muscles and compressing the discs.
2. Can losing weight really stop the need for a knee replacement?
In early to moderate stages of Osteoarthritis, weight loss combined with muscle strengthening can reduce pain so significantly that surgery can be delayed for years or avoided entirely.
3. What is the “Thin-Fat” phenotype?
It refers to people who have a normal weight but a high percentage of body fat and low muscle mass. This is very common in India and increases the risk of joint pain and diabetes.
4. How does obesity affect my eyesight?
Obesity leads to high blood pressure and diabetes, both of which damage the small blood vessels in the retina, leading to conditions like Diabetic Retinopathy.
5. Is walking 10,000 steps good for an obese person with knee pain?
Not necessarily. If your joints are misaligned, 10,000 steps might cause more inflammation. We recommend low-impact strengthening first to support the joint.
6. What are “Adipokines”?
They are inflammatory chemicals released by fat cells that can travel to joints and eyes, causing tissue damage and slowing down healing.
7. Why do you recommend high protein for weight loss?
Protein helps you lose fat while keeping your muscle. Without muscle, your joints have no support, and your metabolism will slow down.
8. Can PRP injections work if I am overweight?
Yes, but they are more effective if you reduce systemic inflammation through weight optimization.
9. What is the risk of “muscle loss” with new weight loss drugs?
Drugs like GLP-1s can cause rapid weight loss, including muscle. This can lead to joint instability if not paired with resistance training.
10. How often should I get my eyes checked if I am overweight?
We recommend a comprehensive eye exam with retinal screening at least once a year if you have metabolic risk factors.
11. Does Move and Shine offer personalized exercise plans?
Yes, our sports medicine team creates customized plans that focus on calorie burning without joint impact.
12. Is “Keto” good for joint pain?
Low-carb diets can reduce inflammation for some, but they must be balanced to ensure you aren’t losing muscle or bone density.
13. What is “Joint Preservation”?
It is a philosophy of using minimally invasive treatments, nutrition, and physiotherapy to keep your natural joints healthy rather than replacing them with metal and plastic.
14. Can obesity cause Glaucoma?
There is a correlation between metabolic syndrome (often caused by obesity) and increased pressure inside the eye, which is a risk factor for Glaucoma.
15. How do I start?
Book a Joint & Metabolic Health Assessment at our clinic. We will look at your movement, your blood markers, and your eye health to create a holistic plan.


