Differentiating Common Shoulder Pain: A Practical Guide for Early Diagnosis and Timely Referral
Shoulder pain has evolved into one of the most clinically challenging musculoskeletal complaints encountered across all age groups. What was once thought to be an issue primarily affecting elderly individuals is now widely observed in athletes, desk professionals, manual laborers, and even adolescents engaged in competitive sports. Despite its frequency, shoulder pain remains one of the most commonly misdiagnosed and mistreated conditions in musculoskeletal medicine.
A major concern in clinical practice is the delay between symptom onset and appropriate specialist intervention. Many individuals initially resort to self-medication, rest, massage therapy, or over-the-counter anti-inflammatory drugs. While these measures may temporarily suppress pain, they do not address underlying structural pathology. In numerous cases, what begins as a simple inflammatory condition progresses into chronic degeneration, tendon retraction, joint stiffness, or instability.
The shoulder is the most mobile joint in the human body. This extraordinary mobility allows activities such as throwing, lifting, reaching, and overhead work. However, mobility comes at the cost of stability. Unlike the hip joint, which benefits from a deep bony socket, the shoulder relies heavily on soft tissue stabilizers — including the rotator cuff, capsule, ligaments, and labrum. When these stabilizers are compromised, dysfunction quickly follows.
For General Practitioners (GPs), physiotherapists, sports medicine professionals, and orthopedic specialists, the ability to differentiate common shoulder conditions is essential. Early structural diagnosis prevents irreversible joint damage and significantly improves long-term outcomes.
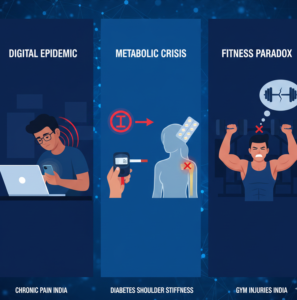
The Modern Clinical Reality of Shoulder Pain
Shoulder disorders today are influenced by three dominant lifestyle factors.
The Digital Posture Epidemic
Prolonged screen exposure has dramatically altered posture mechanics. Forward head posture combined with rounded shoulders reduces the subacromial space — the narrow corridor through which the rotator cuff tendons pass. Chronic narrowing causes mechanical impingement of the supraspinatus tendon and subacromial bursa.
Over time, repeated micro-trauma leads to:
- Tendon degeneration
- Bursal inflammation
- Partial-thickness cuff tears
- Painful arc syndrome
Without correction of biomechanics, impingement can progress to full-thickness rotator cuff tears.
The Metabolic Influence on Soft Tissue
Metabolic disorders affect connective tissue elasticity. Elevated blood glucose leads to collagen cross-linking and capsular fibrosis. Clinically, this manifests as Adhesive Capsulitis (Frozen Shoulder).
The hallmark feature is progressive stiffness, particularly external rotation limitation. Pain often precedes stiffness but may subside while restriction worsens.
If untreated, frozen shoulder can pass through:
- Freezing phase (pain dominant)
- Frozen phase (stiffness dominant)
- Thawing phase (gradual recovery)
However, delayed intervention may prolong this process significantly.
The Fitness Paradox
An increasing number of recreational athletes participate in high-intensity workouts without adequate shoulder conditioning. Poor scapular stabilization combined with heavy overhead lifting predisposes individuals to:
- SLAP tears
- Bankart lesions
- Labral fraying
- Internal impingement
Improper rehabilitation after ligament injuries further increases meniscal and labral complications.
2. The Burden of Shoulder Pain
Shoulder pain consistently ranks among the top musculoskeletal complaints globally. Its burden extends beyond discomfort — it significantly affects daily living, work productivity, athletic performance, and sleep quality.
Occupational Patterns
Desk-Based Professionals
- Impingement syndrome
- Bicipital tendinitis
- Cervico-scapular dysfunction
Manual Laborers
- Repetitive strain injuries
- Degenerative cuff tears
- Post-traumatic instability
Gender-Based Trends
Females demonstrate higher incidence of adhesive capsulitis and autoimmune-related stiffness. Hormonal influences play a role in collagen integrity.
Males more frequently present with:
- Traumatic dislocations
- Contact sports injuries
- Acute cuff tears
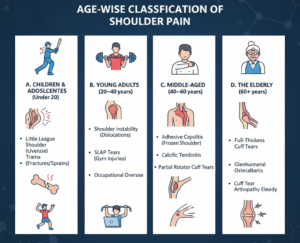
3. Age-Wise Classification of Shoulder Pain
Age remains the most reliable initial diagnostic filter.
A. Children & Adolescents (Under 20 Years)
Degenerative tears are rare.
Common causes include:
- Traumatic instability
- Growth plate stress injuries
- Clavicle fractures
Overhead athletes may develop epiphysitis due to repetitive strain.
B. Young Adults (20–40 Years)
This is the peak age group for instability.
Common conditions:
- Anterior shoulder dislocation
- SLAP tears
- Bankart lesions
- Occupational bursitis
Failure to repair labral damage increases recurrence risk and glenoid bone loss.
Expert Comment – Dr. Pradeep Kochappan
“In the Indian middle-aged population, we must have a high index of suspicion for diabetes. A ‘Frozen Shoulder’ is often the first clinical sign of undiagnosed Type 2 Diabetes. We don’t just treat the shoulder; we screen the system. Preserving the integrity of the rotator cuff in this age group is vital because a repair at age 50 has a much higher success rate than a salvage procedure at age 70.”
C. Middle-Aged Adults (40–60 Years)
Degenerative changes begin.
Common presentations:
- Frozen shoulder
- Calcific tendinitis
- Partial rotator cuff tears
- Painful arc syndrome
Delayed management may convert partial tears into full-thickness tears.
Shoulder Pain After 50: Understanding Rotator Cuff Tears and Arthroscopic Double-Row Repair
D. Elderly (60+ Years)
Common conditions:
- Full-thickness cuff tears
- Glenohumeral osteoarthritis
- Cuff tear arthropathy
Degenerative tears may remain asymptomatic until minor trauma triggers acute symptoms.
4. High-Risk Patient Groups
Certain individuals require aggressive evaluation.
- Diabetic patients with progressive stiffness
- Post-stroke patients with hemiplegic shoulder subluxation
- Athletes with persistent instability
- Cervical radiculopathy patients
Cervical spine pathology can mimic rotator cuff pain. Differentiation is critical.
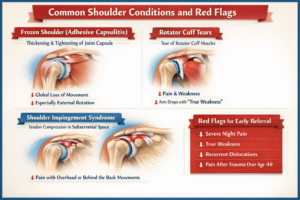
5. Common Shoulder Conditions and Their Clinical Features
Frozen Shoulder
- Global movement restriction
- Capsular thickening
- Severe external rotation limitation
Rotator Cuff Tears
Symptoms:
- Lateral arm pain
- Weakness
- Night pain
- Drop arm sign
Full-thickness tears do not heal spontaneously and may retract over time.
Shoulder Impingement Syndrome
- Painful arc
- Subacromial inflammation
- Pain with overhead activity
Red Flags for Immediate Referral
- Night pain affecting sleep
- Objective muscle weakness
- Recurrent instability episodes
- Trauma-related pain after 40
Shoulder Pain Relief & Prevention | Dr. Viresh Murugodi at Move and Shine Clinic
6. Structured Diagnostic Approach
History
- Trauma history
- Gradual onset
- Systemic disease
Examination
Passive vs Active ROM:
- Passive restricted → Capsular pathology
- Passive full, active limited → Tendon tear
Imaging
- X-ray for bone pathology
- MRI for soft tissue evaluatio
7. Clinical Decision Pathway
Step 1: Age assessment
Step 2: Trauma evaluation
Step 3: Functional testing
Step 4: Imaging
Step 5: Conservative vs surgical decision
Structured rehabilitation for 4–6 weeks if no red flags.
8. When Conservative Management Should Stop
Continued physiotherapy without structural diagnosis can worsen outcomes.
Referral required if:
- Recurrent instability
- Full-thickness tear suspected
- Progressive stiffness
- Post-operative complications
Delayed surgery leads to fatty infiltration and tendon retraction.
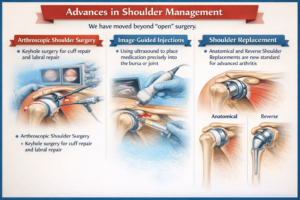
9. Advances in Shoulder Management
Arthroscopy offers reduced morbidity and faster recovery compared to open surgery.
Expert Comment – Dr. Viresh Murugodi
“A common mistake is treating every stiff shoulder as ‘Frozen Shoulder.’ If you aggressively stretch a shoulder with a partial rotator cuff tear, you can convert it into a full-thickness tear. Structural diagnosis must precede mechanical therapy. If a patient is not improving after 4 weeks of structured rehab, it is time to re-evaluate with an MRI.”
10. Long-Term Prevention and Shoulder Preservation
Preventive strategies are essential for long-term joint health.
- Postural correction
- Scapular strengthening
- Rotator cuff conditioning
- Controlled overhead loading
- Proper sports warm-up
Early intervention preserves cartilage integrity and delays osteoarthritis.
11. Comprehensive Patient FAQs
- When should shoulder pain not be ignored?
If it persists for more than 2 weeks, keeps you awake at night, or if you feel the arm is “weak.”
- Is X-ray enough for shoulder pain?
X-ray is excellent for bones and arthritis but cannot see “soft tissue” like the rotator cuff or labrum.
- Can physiotherapy worsen shoulder problems?
Yes, if the therapist is stretching a torn tendon or an unstable joint.
- How long does frozen shoulder last?
In India, without treatment, it can take 18-24 months to resolve. Specialist care can reduce this to weeks.
- When does surgery become unavoidable?
In full-thickness tears, recurrent dislocations, or bone-on-bone arthritis.
- Can I drive with shoulder pain?
Only if it doesn’t impair your ability to make sudden steering maneuvers.
- Is heat or ice better for the shoulder?
Ice for acute injury/inflammation; heat for chronic stiffness.
- What is a “Shoulder Replacement”?
Replacing the damaged joint surfaces with metal and plastic components.
- Why does my shoulder click?
Clicking can be harmless “gas bubbles” or a sign of a labral tear or bursitis.
- Can diabetes cause shoulder pain?
Yes, it is the leading cause of stiff (frozen) shoulders in India.
- What is a SLAP tear?
A tear of the top part of the labrum where the biceps tendon attaches.
- Are steroid injections safe?
One or two targeted injections are safe and effective; repeated injections can damage the tendon.
- Can cervical spondylosis cause shoulder pain?
Yes, nerve compression in the neck often “radiates” to the shoulder.
- How do I sleep with shoulder pain?
Try sleeping on your back or the opposite side with a pillow tucked under the painful arm.
- What is “calcific tendinitis”?
Calcium buildup in the tendon, often causing the most severe “non-injury” shoulder pain.
- Can I play cricket with a labral tear?
Throwing/bowling with a tear can lead to further joint damage and instability.
- Is a “Reverse Shoulder Replacement” different?
Yes, it’s designed for patients with arthritis and a non-functional rotator cuff.
- Can I prevent shoulder pain?
Yes, through posture correction, scapular exercises, and avoiding sudden heavy overhead lifts.
- How long is the recovery after cuff surgery?
Usually 6 months for a full return to high-level activity.
- Who is a “Shoulder Specialist”?
An Orthopedic Surgeon who has undergone specific fellowship training in shoulder arthroscopy and replacement.
Why Persistent Shoulder Pain Should Not Be Ignored: Early Warning Signs and Structural Causes
12. Conclusion
The management of shoulder pain requires early structural differentiation. Accurate diagnosis determines whether conservative care, injection therapy, or surgical repair is required.
A painful or stiff shoulder is not merely discomfort — it may signal structural compromise that demands timely intervention.
Prompt specialist evaluation preserves joint function, prevents irreversible degeneration, and restores long-term mobility.


